Some hypothyroid patients continue to exhibit symptoms even while they are treated with the appropriate doses of levothyroxine (L-T4). Over 10 million Americans suffer from hypothyroidism, thus the number of dissatisfied patients is not small.
Recent studies show that the answer might be on how some hypothyroid patients metabolize L-T4. After reaching the bloodstream, T4 must be activated to T3 to regulate metabolism. However, studies in Europe and the US have shown that L-T4-treated hypothyroid patients do not produce normal amounts of T3, even when their TSH levels in the blood are normal. Physicians have long attempted to fix this problem by prescribing treatment with a combination of L-T4 + L-T3, in order to fully restore blood levels of T3. However, treatment with L-T3 is complicated by a T3 spike in the blood 3-4 hours after patients take the tablets. Some patients experience palpitation, tightness of the chest and sweating; no long-term safety studies are available for patients taking L-T3.
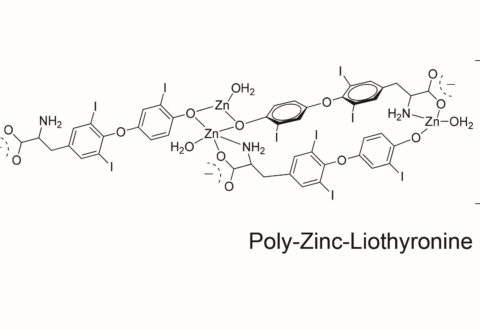
To remedy this problem, a metal coordinated form of L-T3, [Zn(T3)(H2O)]n known as poly-zinc-liothyronine (PZL), was synthesized, loaded into capsules and tested in hypothyroid rats. The results were exciting. Rats receiving PZL absorbed LT3 at a much slower rate, resulting in less fluctuation of blood T3 levels over time. This is because contrary to L-T3, PZL is broken down in the intestine and slowly releases L-T3 for absorption into the bloodstream. Notwithstanding a much slower rate of absorption, treatment with PZL resulted in similar long-term effects towards correcting the hypothyroidism.
The authors of the study concluded that capsules of PZL given orally normalize bodily processes that are T3-dependent while exhibiting a reduced and delayed spike of T3 in the blood. This provides a longer period of relatively stable serum T3 levels when compared with capsules of L-T3. Future clinical trials should determine whether these enhanced properties might render PZL a more suitable pharmaceutical to normalize circulating T3 levels in L-T4-treated hypothyroid patients.
Contributed by Rodrigo da Conceicao PhD
Original studies at: PMID: 30301431